I want to elaborate on a couple of topics not previously addressed:
- If the brain is so full of DHA, then why does EPA (and not DHA) help with mood*?
- The concept of ‘Unopposed EPA’
The best summary of the state of the science was published by Dr. Sublette of Columbia University Medical Center. She also has a website called MoodStudies.org
Dr. Sublette found that mood was significantly improved when a fish oil formula had 60% or more EPA.*
*Individual results will vary. These statements have not been evaluated by the Food and Drug Administration. This product is not intended to diagnose, treat, cure, or prevent any disease. Research suggests that improving omega-3 fat intake from a concentrated source may help support a healthy mood. Some, but not all studies, indicate that 2,000 mg of omega-3 fats daily with a higher concentration of EPA may offer benefit.
If the fish oil contained equal parts EPA and DHA or mostly DHA, there was no improvement.
Actually, DHA is contraindicated for mood per this publication.
But this flies in the face of two facts:
- DHA is the major component of the brain – there is hardly any EPA in the brain
- People with poor mood health have less DHA in their brain
So…what gives?
We don’t have all the answers yet, but here are a few possible reasons:
-
Mood may not be just brain-related*
- We think of mood as being exclusively brain-related. I’ve argued that mood health is partly gut-and-diet related. If you eat crap (sugar, wheat & vegetable oils), then your gut may become leaky and, well, moody.
- The concept of the gut-brain axis is still fairly new to western medicine. Progress is slow. Our grandchildren will hear a lot more about it than we do. Listen to Chris Kresser talk about it on his podcast.
- Makes you rethink the term ‘gut feeling,’ doesn’t it?
-
EPA possibly enters brain and improves function*
- Just because there is very little EPA in the brain does not mean it is not absorbed and/or rapidly used up (rapid turnover.)
- We know this happens in mice. No proof yet if it happens in people – wanna volunteer?
- EPA supplementation increases N-acetyl aspartate, a marker of nerve health and phospholipid turnover.*
- EPA supplementation supports brain health*
-
EPA indirectly increases DHA levels in the brain
- EPA is a precursor to DHA.
- EPA could increase production of DHA but the evidence here is weak.
-
Mood health is likely a symptom of other conditions*
- This may be the most important of the four points…mood health may simply be a symptom of poor inflammation response.
- We already talked about EPA and its preventive role in supporting health inflammation response*.
- Read ‘Cytokines sing the blues’ by Raison et al., 2006. .
But there’s more!
- Ratios of Omega-6 to 3 are increased in the people with poor mood health (never hurts to flog that dead horse!)
- Our bodies make serotonin (the happy chemical) from tryptophan. But if you’re unwell, your body will convert tryptophan into agitation-causing molecules (kynurenic and xanthurenic acid.) Groovy diagram explains this.
OK, but why does excess DHA not help?
The Sublette paper suggests it could be due to EPA and DHA competing for some unknown binding site where EPA in excess helps and DHA in excess hurts. And Maes et al., says it could be because DHA induces a Th-1-like immune response, which makes DHA contraindicated for mood health. (I’d love to explain that but it’s above my pay grade. 🙂 And I like being awake. Thanks for asking.)
What is Unopposed EPA?
The concept of unopposed EPA comes from the understanding that fish oil formulas that contained 60% or more EPA support mood health*.
The higher the percent of EPA in the formula, the more likely it was to help.
So if your fish oil supplement contains 500 mg total Omega-3, of which 300 mg is EPA and 200 mg is DHA, then the unopposed EPA = mg EPA minus mg DHA. 300 – 200 = 100 mg of unopposed EPA.
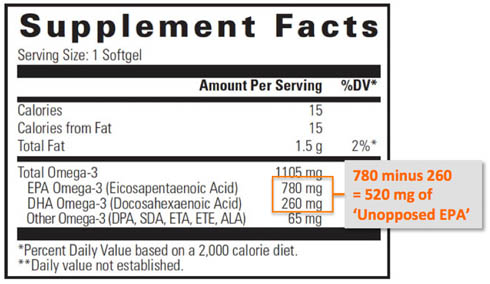

More is not better. Again.
Don’t gulp down 20 fish oil pills after reading all this.
Turns out, there is a sweet spot: between 1000 mg and 2200 mg of unopposed EPA per day. One study noticed benefits with just 200 mg of unopposed EPA per day.
Too much unopposed EPA, and no benefit.
Poor mood health can have many causes. Taking EPA may not have much effect if your mood health is driven by factors unrelated to Omega-3, such as emotional/psychological factors.
*Individual results will vary. Nutritional therapy may only help support positive mood if poor nutrition (and associated deficiencies) was a preexisting condition. These statements have not been evaluated by the Food and Drug Administration. This product is not intended to diagnose, treat, cure, or prevent any disease. Research suggests that improving omega-3 fat intake from a concentrated source may help support a healthy mood. Some, but not all studies, indicate that 2,000 mg of omega-3 fats daily with a higher concentration of EPA may offer benefit.


Hi Karim – you’d be fine with a regular ratio since you’re primarily brain focused. But remember, fish oil + bad diet = bad diet. You may get greater benefits from switching to a whole foods only diet.
OmegaVia is certainly NOT the only option available to you. Experiment with both supplement and diet and see what works best. But definitely avoid Omega-6 supplements!
I am watching my diet and also trying to get a boost from a fish oil supplement.
Which is more important to me EPA or DHA ?
I have been reading all these research papers since yesterday and I am simply lost 🙂
Is taking a supplement with high EPA cancel the benifits of the DHA (“unopposed “DHA =0)
sorry for asking all these questions but I am just trying to get the best thing for my condition.
Karim – a high EPA product would be better for you. But if you can’t find one, don’t over-think it. Just go with what you can find. That’s Step 1. Unless you like reading and interpreting research papers, it will probably send you in too many directions.
I really appreciate you spending time sharing your experience with people you don’t even know !
If EPA is better for me ,I’ll go with Omegavia as 2 pills provide at least 1040 mg EPA and still get a fair amount of DHA.
Thank you very much .
You’re welcome.
Shop around the periphery of the grocery store where the fresh, whole foods are. Nothing in the middle of the grocery store in boxes, bags and containers – those are delicious food-like substances, not real food. Eat eggs, liver, seafood, green leafy veggies, fermented foods, healthy fats, grass-fed meats, a few nuts and fruits as dessert. Other than nuts, everything should have been alive a few days ago. If not, you’re eating the wrong thing.
Yes, assuming your depression was caused by Omega-3 deficiency. I know a couple of doctors who’ve put their patients on Vascepa for depression. That’s why we recently introduced this product: http://www.amazon.com/OmegaVia-Pharmaceutical-EPA-Only-Burp-Free-Mini-Gels/dp/B00D37S0HC/
Of course, there are a dozen other nutritional factors and some non-nutritional ones that cause or contribute to depression. True relief from depression requires addressing most (if not all) of those issues. Sometimes, it’s not just including some nutrients in your diet but eliminating other toxic ones like gluten that will bring relief.
Vin – 1000 mg of epa sounds good but how much of it is absorbed? I’ve read that even though Krill oil has much smaller amounts of epa – it is absorbed 10 times better than fish oil which,if true, means that the large amounts of fish oil actually add up to less being absorbed than a much smaller amt. of Krill oil? Please help – I am confused – thanks – Locke
Hi Locke – yes, 1000 mg of EPA should be fine for most people. Absorption is not a problem with any of the Omega-3s, especially if you take your Omegas with a meal. This doubt has, sadly, been injected into the public discourse by self-serving marketing folks selling one product or another. The superiority of krill oil has been established – it is about 1.6 times better absorbed than fish oil. More on that here: http://www.omegavia.com/is-krill-oil-48x-better-than-fish-oil/ So, yes, krill oil is a little better. To get the same effect of 1000 mg of fish-derived EPA, you’d only have to take 625 mg of EPA from krill. But given that most krill oil pills have less than 100 mg EPA per pill, you’d have to take about 8 pills a day.
Hi Joe – your dose for triglyceride reduction should accomplish both tasks…assuming your mood issues are Omega-3 related, of course.
Hi Julie – emotional and psychological factors are often, but not the only, causes for mood and sleep issues. People need professional help to address both, psychological and physical issues. EPA is merely a partial solution to one of the physical issues.
Hi. Where do you stand on adding Griffonia supplements to a daily omegavia intake? Thank you.
Hi Rory – I am not aware of a reason why you cannot take Griffonia with OmeagaVia. Griffonia is a plant source of 5-HTP. And 5-HTP can get converted to Serotonin, a happy chemical. Given how simple that may seem, the science is not compelling enough to support the use for mood support. In rodent studies, yes, but surprisingly, not yet in humans. If your diet is deficient in Tryptophan, 5-HTP may be an option. But the easier thing to do is increase consumption of higher quality proteins. Also, if you have chronic inflammation from metabolic disorder, your body can quickly process out Tryptophan, leaving you with less substrate for Serotonin production. Metabolic disorder is a medical condition that you will need your doctor’s attention. Fortunately, Metabolic disorder also responds extremely well to exercise, healthy diet, and lifestyle alterations. If you’re interested in nutrients that influence mood, take a look at this page.
I’m
Having trouble finding a pure epa supplement in australia ( I want to try 1000mg per day for depression ) – I’ve read above about available epa when taking a supplement that also contains dha.
So- Is 1000 mg of EPA in a pure EPA supplement as affective as taking a combination EPA/DHA supplement with the available EPA is 1000 mg – does the DHA somehow render the EPA less effective ?
Or any referral to a pure epa supplement also appreciated .
Thanks .
Hi Ilhas – depression can have non-nutritional causes (social, physical, emotional etc.) that may require professional treatment.
Having said that, providing your body with nutrients like EPA, Vitamin D3, B-vitamins, magnesium, combined with herbs like Curcumin can help the body produce the healthy levels of neurotransmitters. Regarding EPA or unopposed EPA, you don’t need to take pure EPA. If your supplement contains 300 mg of EPA and 100 mg of DHA, you are getting 200 mg of unopposed EPA. Studies are starting to show that 1000 to 2000 mg of unopposed EPA may help with mood. You can get that much unopposed EPA with fewer pills if you use an EPA-rich or EPA-only supplement. Or you can get there with regular fish oil but with more pills.
If I were you, I’d start with any available Omega-3 supplement with a target of 2000 to 3000 mg of total Omega-3 and hope you get about 1000 mg of unopposed EPA from it.
FYI – we ship our EPA 500 to Australia.